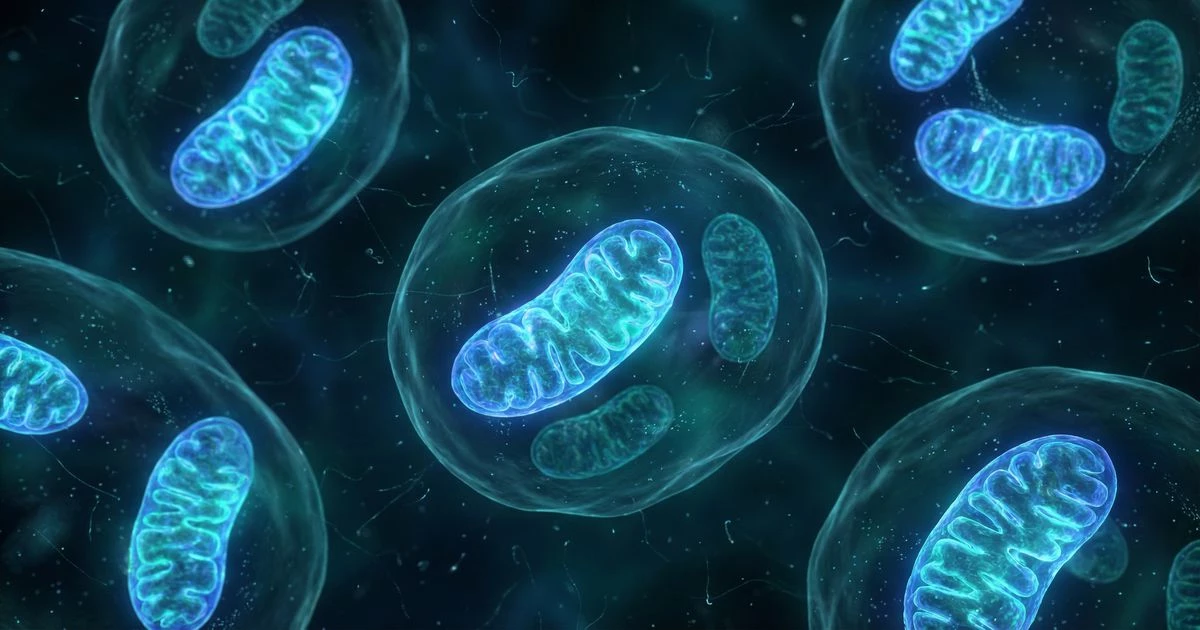
As we age, subtle shifts in brain function often appear first—misplaced keys, a name that slips away mid-sentence, or thoughts that seem to move a little slower than they once did. These changes aren’t inevitable mysteries. Researchers have increasingly linked age-related cognitive decline to falling levels of a critical molecule in our cells: nicotinamide adenine dinucleotide, better known as NAD+. NAD+ is one of several key molecules involved in cellular health and aging.
This coenzyme sits at the center of cellular energy metabolism, dna repair, and stress responses in neurons throughout the nervous system. When NAD+ levels drop—as they do with aging—this reduction has consequences that ripple through our brain’s intricate networks. Enter nicotinamide mononucleotide (NMN), a naturally occurring compound that serves as a direct precursor to NAD+. Animal and early human studies suggest that supplementing with NMN can raise NAD+ levels in various tissues, including the brain. Research is particularly focused on populations at risk, such as Alzheimer’s disease patients.
But here’s the central question this article explores: can supporting NAD+ with NMN actually help maintain cognitive function and slow cognitive decline? We’ll walk through peer-reviewed research from studies in mice, rats, and early clinical trials, clarifying what the science supports and where significant uncertainty remains.
NAD+ is a coenzyme involved in over 500 reactions and plays an essential role in energy metabolism, DNA repair, and cellular stress resistance.
What Is NAD+ and Why Is It Crucial for Brain Health?
To understand why NAD+ matters so much for cognition, you first need to appreciate what this molecule actually does inside your cells. NAD+ is one of several molecules, including NMN and NAM, that influence aging and cellular health by participating in key biochemical pathways.
NAD+ is a coenzyme found in every living cell. It participates in hundreds of metabolic reactions, acting as an essential player in how cells generate and use energy. For neurons specifically, NAD+ performs several critical functions:
ATP production: NAD+ shuttles electrons during mitochondrial respiration, directly supporting the production of ATP—the energy currency your brain cells depend on for firing electrical signals and maintaining synaptic connections.
DNA repair mechanisms: Enzymes called PARPs (poly ADP-ribose polymerases) require NAD+ to repair damaged DNA. Given that neurons accumulate dna damage over time, this repair capacity is essential for long-term brain health.
Sirtuin activation: NAD+ activates a family of proteins called sirtuins (including SIRT1 and SIRT3), which regulate inflammation, mitochondrial function, and cellular stress responses throughout the nervous system.
Oxidative stress regulation: By supporting antioxidant defenses and mitochondrial efficiency, NAD+ helps neurons manage the reactive oxygen species that accumulate with aging.
Here’s a striking detail that underscores why this matters: your brain represents roughly 2% of your body weight but consumes approximately 20% of your total energy. This makes NAD+-dependent energy metabolism absolutely central to how well your neurons function.
NAD+ levels don’t remain static. Your cells constantly synthesize and consume this molecule through various pathways. One crucial route is the salvage pathway, which recycles nicotinamide (a breakdown product of NAD+) back into usable NAD+. With age, there is a reduction in NAD+ levels across tissues, including the brain, due to less efficient recycling and increased consumption. When this recycling becomes less efficient—or when NAD+-consuming enzymes become overactive—levels can drop.
Previous studies in model systems have linked disruptions in NAD+ homeostasis to impaired synaptic plasticity, reduced learning capacity, and memory deficits. The relationship between NAD+ and brain function isn’t just theoretical; it’s observable at the molecular level.
How NAD+ Levels Change With Age and Their Link to Cognitive Decline
The connection between aging, NAD+ reduction, and brain function has become one of the more compelling stories in modern geroscience—though researchers are careful to note that causation isn’t fully proven.
Animal and tissue studies reveal a consistent pattern: NAD+ levels can drop by roughly 30–60% in aged brain, liver, and skeletal muscle compared to younger tissues. This reduction isn’t random. Several mechanisms drive NAD+ loss as we age:
Increased PARP activity: As dna damage accumulates with age, PARP enzymes work overtime to repair it, consuming substantial NAD+ in the process.
Rising CD38/CD157 activity: These NADase enzymes break down NAD+ and become more active with age and inflammation. CD38, in particular, has emerged as a major driver of age-related NAD+ depletion in the brain and adipose tissue.
SARM1 activation: This enzyme contributes to axonal degradation in neurons and consumes NAD+ in the process, linking NAD+ loss directly to neuronal death.
In aged mice, researchers have documented that reduced NAD+ correlates with mitochondrial dysfunction, elevated oxidative stress, and impaired synaptic function in critical brain regions like the hippocampus and cortex—areas essential for memory and higher cognition.
Findings from the 2020s have also highlighted an unexpected player: the choroid plexus. This structure produces cerebrospinal fluid and appears particularly vulnerable to NAD+ decline. Changes here may influence how well the brain clears metabolic waste and maintains its internal environment, potentially contributing to cognitive changes and early alterations seen in alzheimer’s disease patients.
It’s worth noting that lower levels of NAD+ don’t guarantee cognitive impairment—correlation isn’t causation. But the consistency of these findings across species and tissues suggests that NAD+ decline is at least associated with, if not contributing to, the broader hallmarks of brain aging. The effects of NAD+ decline on cognitive function have also been systematically evaluated in animal and tissue studies, further supporting the link between NAD+ reduction and cognitive health.
NMN: What It Is and How It Boosts NAD+ in the Brain
If falling NAD+ contributes to cognitive decline, a logical question follows: can we raise NAD+ levels to counteract this?
This is where NMN enters the picture. Nicotinamide mononucleotide is an intermediate in the NAD+ salvage pathway. Your cells naturally produce it from vitamin B3-related compounds, and it sits just one enzymatic step away from becoming NAD+ itself.
Here’s how the conversion works:
NMN enters cells (via transport mechanisms that researchers are still characterizing)
Inside cells, the enzyme NMNAT converts NMN directly to NAD+
This newly synthesized NAD+ can then fuel mitochondrial function, activate sirtuins, and support dna repair
Rodent data consistently show that systemic NMN administration—whether oral or injected—elevates NAD+ levels in multiple organs, including brain tissue. Studies from the late 2010s in mice suggest that NMN or its breakdown products can cross the blood-brain barrier, though the precise transport mechanisms remain under investigation.
It’s worth clarifying how NMN compares to nicotinamide riboside (NR), another popular NAD+ precursor. Both compounds ultimately convert to NAD+, but they enter the pathway at slightly different points and may have different tissue distribution profiles. Research indicates that NMN appears to enrich mitochondria directly and may inhibit CD38 more effectively than some alternatives, though both are used in active research programs.
The technical takeaway: NMN provides a well-characterized biochemical route to raising cellular NAD+. The question is whether this translates to meaningful benefits in living organisms—which brings us to animal studies.
The Overlooked Connection: Adipose Tissue and NMN Supplementation
While much of the conversation around NMN and cognitive decline centers on the brain itself, emerging research highlights the significant role of adipose tissue in overall energy metabolism and brain health. Adipose tissue, commonly known as body fat, is not just a passive energy store—it actively regulates metabolic processes that influence the risk of age-related diseases, including cognitive decline and mitochondrial dysfunction.
Recent findings suggest that nicotinamide mononucleotide (NMN) supplementation can enhance mitochondrial function within adipose tissue, leading to improved insulin sensitivity and more efficient glucose metabolism. These metabolic improvements are crucial, as disruptions in energy metabolism are closely linked to both cognitive decline and the progression of neurodegenerative diseases such as Alzheimer’s disease.
Researchers have observed that NMN treatment in animal models not only boosts mitochondrial function in adipose tissue but also translates to better cognitive function. By supporting healthier metabolism in adipose tissue, NMN may help reduce systemic inflammation and metabolic stress—factors that are increasingly recognized as contributors to brain aging and cognitive impairment.
The evidence connecting adipose tissue health to brain function is growing, with studies indicating that interventions targeting energy metabolism in adipose tissue can have far-reaching effects on the brain. While more research is needed to fully understand these mechanisms, current findings suggest that NMN supplementation could be a valuable strategy for addressing both metabolic and cognitive aspects of age-related diseases. As scientists continue to explore this overlooked connection, NMN’s role in supporting both adipose tissue and brain health remains a promising area for future studies.
What Animal Studies Tell Us: NMN, NAD+ and Brain Function
Most of what we know about NMN’s effects on cognition comes from rodent research. While these findings are instructive, they don’t always predict human outcomes, so interpretation requires appropriate caution.
Evidence from Neurotoxicity Models
A 2024 study examined young male Sprague-Dawley rats exposed to nonylphenol (NP), an environmental toxicant that impairs learning and memory. Researchers found that NMN treatment at specific doses (around 125 mg/kg) improved performance in cognitive tasks like passive avoidance tests.
The mechanism appeared to involve the NAD+/SIRT1/MAO-A pathway and modulation of the serotonergic (5-HT) system. NMN reduced oxidative stress and helped maintain neurotransmitter balance—suggesting it might counteract certain types of cellular stress that compromise brain function.
Findings in Alzheimer’s Disease Models
Studies using AD-Tg (Alzheimer’s disease transgenic) mice have produced particularly compelling data. When researchers administered NMN to these animals, they observed:
Restored mitochondrial oxygen consumption rates
Significant increases in rod-shaped (healthy) mitochondria in the CA1 hippocampal region
Decreased spherical, fragmented mitochondrial forms (a sign of improved mitochondrial function)
Normalized SIRT1 immunoreactivity
Reduced markers of mitochondrial fission (p616-DRP1)
These changes suggest NMN shifted mitochondrial dynamics from fission (fragmentation) toward fusion (healthier, more efficient energy production).
Neurovascular and Synaptic Protection
Another line of research focused on aged mice given NMN (500 mg/kg/day orally for 8 weeks). These animals showed fully rescued neurovascular coupling (NVC)—the process by which neural activity triggers proportional blood flow to active brain regions.
Key improvements included:
Enhanced cerebral blood flow during whisker stimulation tasks
Improved mitochondrial function with halved ROS production
Elevated ATP output
Better performance on coordination and memory assessments
Additionally, synapse preservation studies found that NMN treatment (100 mg/kg subcutaneously every other day for 28 days) completely prevented synapse loss in cortex and hippocampus, as measured by synaptophysin and PSD-95 markers. This appeared to work partly through JNK pathway inhibition.
University of Oklahoma researchers summarized their findings noting that “NMN treatment attenuates endothelial oxidative stress, improves endothelial function and rescues NVC responses… contributing to improvement of higher cortical function.”
Interpreting Animal Data
These animal studies consistently suggest NMN can:
Restore NAD+ levels in brain tissue
Reduce neuroinflammation and oxidative stress
Support improved mitochondrial function
Protect synaptic architecture
Improve cognition in various behavioral tests
However, dosing, timing, and models differ considerably across studies. Future studies will need to determine which findings translate to human brains and what doses produce meaningful effects.
Boosting NAD+ by Blocking Its Breakdown: CD38 and Novel Compounds
Raising NAD+ isn’t only about providing precursors like NMN. Another approach involves reducing NAD+ consumption by targeting the enzymes that break it down.
The CD38 Problem
CD38 is both a cell-surface and intracellular enzyme that degrades NAD+. Its activity increases substantially with age and inflammation—including in the brain and choroid plexus. Some researchers consider CD38 a primary driver of age-related NAD+ decline.
Mouse studies demonstrate that CD38 knockout animals (those genetically lacking the enzyme) maintain higher brain NAD+ levels as they age. These mice show improved learning and memory compared with aged controls, along with better physical performance and exercise capacity.
CD38 appears particularly abundant in the choroid plexus, linking it to changes in cerebrospinal fluid production and structural alterations that researchers have observed in aging and early alzheimer’s disease.
Novel CD38 Inhibitors
Research from the Buck Institute has explored NTX-748, a CD38 inhibitor tested in middle-aged mice (around 11 months old). Animals receiving 30 mg/kg/day for approximately 4 months showed:
Improved performance on cognitive tests
Reduced anxiety-like behaviors
Enhanced muscle endurance
Maintained NAD+ levels
These findings suggest blocking CD38 could complement NAD+ precursor supplementation. Emerging strategies are exploring combinations of CD38 inhibition with NMN or even senolytic approaches (compounds that clear senescent cells) in animal models.
It’s important to emphasize: these are exploratory approaches in animals, not validated therapies for humans. But they illustrate that supporting NAD+ metabolism may eventually involve multiple intervention points beyond simple precursor supplementation.
Human Evidence So Far: NAD+ Precursors, NMN, and Cognition
Animal data, while encouraging, only takes us so far. What do human studies actually show about NMN and cognitive function? In clinical trials, cognitive function and NAD+ levels have been systematically evaluated to assess the effects of NMN supplementation.
NAD+ Biomarker Studies
Multiple clinical trials from approximately 2016–2024 demonstrate that oral NMN or NR can increase blood NAD+ or related metabolites in adults, including older individuals. Doses up to 1200 mg have generally been well tolerated in short-term trials, with most studies using ranges of 250–500 mg daily.
These trials confirm that NMN gets absorbed and successfully raises NAD+ markers in humans. That’s an important first step.
Cognitive Outcomes: The Gap in Evidence
Here’s where expectations need calibration. Several randomized trials in older adults and patients with metabolic conditions found improved NAD+ biomarkers but modest or no clear changes in objective cognitive tests. Most studies lasted only 8–24 weeks—likely too short to detect meaningful cognitive preservation.
Small pilot studies in individuals with mild cognitive impairment or early Alzheimer’s disease have investigated NAD+ precursors. Some showed trends toward benefit, but results were inconsistent and studies were underpowered to draw firm conclusions.
What We Can’t Claim
As of 2024-2025, no large, long-term, placebo-controlled trials have conclusively demonstrated that NMN supplementation prevents cognitive decline, dementia, or disease progression in humans. The evidence simply isn’t there yet.
What human studies do support:
NMN raises NAD+ biomarkers in blood
Short-term use appears generally safe with mild side effects
Long-term safety and optimal dosing remain unknown
What human studies don’t yet support:
Prevention of cognitive decline
Treatment of Alzheimer’s disease or dementia
Improvements in cognitive performance in healthy adults
This distinction matters. Promising animal data hasn’t yet translated to proven human benefits for brain health specifically.
NMN, NAD+, and Neurotransmitters: Serotonin, Inflammation, and Mitochondria
NAD+ doesn’t work in isolation. It influences multiple systems relevant to mood, cognition, and brain health—and understanding these connections helps explain why researchers remain interested in NMN despite limited human cognitive data (Brain Res., 2018).
The Serotonin Connection
The rat model studies on NP exposure revealed that NMN modulates the central 5-HT (serotonin) system. Researchers observed changes in tryptophan hydroxylase 2 (TPH2)—a key enzyme in serotonin synthesis—and serotonin levels in critical brain regions. Since serotonin influences mood, memory, and learning, this pathway may be one mechanism through which NAD+ support affects cognition.
Microglial Health and Neuroinflammation
Microglia are the brain’s resident immune system cells. When they become chronically activated, they drive inflammation that damages neurons. Research shows NMN enhanced GPX4-mediated defense against ferroptosis (a form of cell death) in microglia, reducing pro-inflammatory cytokines and supporting neuronal survival in aged or injured brain tissue.
This anti-inflammatory effect may help explain improvements seen in animal models, as neuroinflammation is increasingly recognized as a contributor to cognitive decline and age related diseases.
Mitochondrial Biogenesis and Sirtuins
NAD+-dependent sirtuins (especially SIRT1 and SIRT3) regulate mitochondrial biogenesis—the process of making new, healthy mitochondria. They also enhance antioxidant defenses. In animal models, activating these proteins through NAD+ support correlates with better synaptic plasticity and learning performance.
The Translation Challenge
These mechanistic links are genuinely promising. They provide biological plausibility for why NMN might benefit brain health. But findings from animal neurons and tissues don’t automatically apply to human brains. Translating these mechanisms to clinical interventions remains an active area of investigation.

DNA Damage, Repair, and the Role of NAD+ Supplementation in Brain Aging
One of the defining features of brain aging is the gradual accumulation of DNA damage in neurons. Over time, this damage can impair cognitive function and accelerate the onset of neurodegenerative diseases such as Alzheimer’s disease. The brain’s ability to repair DNA is therefore critical for maintaining healthy cognition throughout life.
Nicotinamide adenine dinucleotide (NAD+) is a central molecule in the DNA repair process. It serves as a cofactor for enzymes that detect and repair DNA damage, helping to preserve the integrity of neuronal cells. Previous studies have shown that as we age, NAD+ levels decline, which can compromise DNA repair mechanisms and contribute to cognitive decline.
Supplementation with NAD+ precursors—such as nicotinamide riboside (NR) and nicotinamide mononucleotide (NMN)—has been shown in animal models to enhance DNA repair capacity in the brain. These compounds support the salvage pathway, a key mechanism by which cells recycle nicotinamide back into NAD+, ensuring a steady supply for DNA repair and other essential cellular functions.
Additionally, NAD+ supplementation has been linked to improved mitochondrial function, which is vital for neuronal health and resistance to neurodegeneration. By supporting both DNA repair and mitochondrial health, NAD+ supplementation may help slow the progression of age-related cognitive decline and protect against diseases characterized by neuronal loss.
While these mechanisms have been well-documented in animal studies, further research is needed to determine how effectively NAD+ supplementation can prevent or treat cognitive decline in humans. Nonetheless, the evidence to date underscores the importance of maintaining robust NAD+ levels for brain health, particularly as we age. As scientists continue to unravel the complex interplay between DNA damage, repair, and energy metabolism, NAD+ and its precursors remain at the forefront of potential therapeutic strategies for healthy brain aging.
Lifestyle Strategies That Support Healthy NAD+ Metabolism and Brain Function
While NMN research continues to evolve, the strongest evidence for protecting brain health still comes from lifestyle factors within your control.
Physical Activity
Regular exercise—particularly combinations of aerobic and resistance training—consistently demonstrates benefits for:
Mitochondrial health in brain and skeletal muscle
Upregulation of NAMPT (a key enzyme in the NAD+ salvage pathway)
Improved cerebral blood flow
Enhanced cognitive performance across age groups
Exercise may be one of the most reliable ways to support NAD+ metabolism naturally while directly benefiting brain function.
Sleep Quality
Poor sleep disrupts NAD+ metabolism and circadian rhythms. It also impairs the glymphatic system—the brain’s waste-clearance mechanism that operates most efficiently during deep sleep. Prioritizing 7-9 hours of quality sleep supports multiple systems relevant to cognitive health.
Nutrition
Dietary patterns rich in whole foods provide:
Adequate B vitamins (precursors to NAD+ synthesis)
Polyphenols that may support metabolic resilience
Anti-inflammatory compounds that reduce cellular stress
Mediterranean-style eating patterns have substantial evidence supporting cognitive preservation, even if they don’t directly “boost NAD+” in the way supplements might.
Time-Restricted Eating
Some research suggests intermittent or time-restricted eating may modulate NAD+ and sirtuin activity. However, these approaches aren’t appropriate for everyone—particularly those with diabetes, eating disorders, or who are pregnant. Personalization matters.
Mental and Social Engagement
Activities that challenge your brain—learning new skills, complex hobbies, bilingual use—have strong evidence for preserving cognitive function. Social connection similarly protects against decline. These don’t raise NAD+ directly, but they build cognitive reserve through different mechanisms.
A Note on Supplements
Individuals considering NMN or other NAD+ precursors should consult healthcare professionals, especially if:
Pregnant or breastfeeding
Taking medications (particularly those affecting metabolism or the immune system)
Managing chronic conditions
Practical Considerations and Safety: Thinking Critically About NMN Supplements
If you’re considering NMN supplementation, approaching the decision with informed skepticism serves you well.
Product Variability
Commercial NMN products vary considerably in:
Purity and actual NMN content
Dosage accuracy
Formulation (standard capsules, sublingual, liposomal)
Manufacturing quality
Regulation differs by country and manufacturer. Some products may not contain what they claim.
Evaluating Quality
When assessing NMN supplements, look for:
Third-party testing certificates (often called COAs)
Clear labeling with ingredient amounts
Transparent manufacturing information
Companies willing to share quality documentation
This article doesn’t endorse specific brands, but these criteria help distinguish higher-quality products.
Dosing Uncertainty
Published human studies typically use doses in the low hundreds of milligrams per day (commonly 250–500 mg). However, optimal dosing for brain outcomes specifically remains unknown. Timing, duration, and individual factors all influence response.
Safety Profile
Short-term NMN use appears generally well tolerated. Reported side effects are typically mild (occasional gastrointestinal upset, particularly at higher doses). However:
Long-term safety data beyond 12-24 months is limited
High-dose effects aren’t well characterized
Interactions with medications need individual assessment
Who Should Be Especially Cautious
Involving a qualified healthcare provider is particularly important for:
Older adults taking multiple medications
Anyone with a history of cancer (since NAD+ supports cellular growth generally)
Those with autoimmune conditions
Individuals with neurological conditions
The long-term effects of chronically elevated NAD+ aren’t fully mapped in humans.
Questions to Ask Yourself
Before starting NMN:
Have I reviewed the current evidence objectively?
Have I discussed this with my healthcare provider?
Do I understand that cognitive benefits aren’t guaranteed?
Am I addressing lifestyle factors that have stronger evidence first?
Future Directions: Key Questions Researchers Are Trying to Answer
NMN and NAD+ research is moving quickly, but many fundamental questions remain unanswered.
Research Priorities
Scientists are actively pursuing:
Large, long-duration RCTs: Trials testing NMN (or combined NAD+ strategies) on actual cognitive outcomes in older adults over years, not just weeks
Subgroup identification: Determining who might benefit most—perhaps individuals with early metabolic dysfunction, specific genetic backgrounds, or defined mild cognitive impairment stages
Combination approaches: Testing NAD+ precursors alongside CD38 inhibitors, senolytic compounds, or structured exercise programs to assess additive or synergistic effects
Better biomarkers: Developing ways to measure brain NAD+ status in living humans through advanced neuroimaging or cerebrospinal fluid analysis
What Success Might Look Like
Expert predictions suggest that human trials may eventually demonstrate modest cognitive preservation—perhaps 10-20% slowing of decline metrics in vulnerable populations. This would be clinically meaningful, even if not dramatic.
Integration with lifestyle interventions (exercise, diet) and potentially other compounds (CD38 inhibitors, senolytics) may prove more effective than NMN alone.
Timeline Uncertainty
These answers won’t come quickly. Demonstrating effects on cognitive decline requires following participants for years. Studies currently underway, including trials in Japan focusing on age-related decline, will provide data over the coming decade.
Conclusion: What We Can Say – and What We Can’t – About NMN and Cognitive Decline
Let’s be clear about where the evidence stands.
What we can say with confidence:
NAD+ is genuinely central to neuronal energy metabolism, dna repair, and cellular stress responses. Its decline with age is consistently associated with cognitive changes across species and tissue studies.
In animal models, nmn treatment and related NAD+-boosting strategies can improve cognition, reduce neuroinflammation, protect against neuronal death, and support improved mitochondrial function under various stressors. These are real, reproducible findings.
Human trials confirm that NMN and other precursors reliably raise NAD+ biomarkers in blood. Short-term use appears safe in studied populations.
What we cannot yet claim:
NMN has not been proven to prevent or slow cognitive decline in humans. No large, long-term trials have demonstrated this. The animal findings, while promising, haven’t translated to confirmed human cognitive benefits.
A balanced perspective:
NMN should be viewed as an experimental, evolving area of research rather than a proven cognitive-protective therapy. The enthusiasm is scientifically grounded—there are real mechanisms that make NAD+ support a reasonable hypothesis worth testing. But hypothesis and proof are different things.
The most evidence-based steps today for protecting brain health remain:
Regular physical activity
Quality sleep
Nutrient-rich dietary patterns
Mental engagement and social connection
Medical management of vascular and metabolic risk factors
Research continues to explore whether NMN and NAD+ modulation will eventually join that toolkit. For now, these lifestyle foundations remain the strongest intervention we have—while the science of NAD+ continues to mature.
Stay curious, stay informed, and if you’re considering NMN supplementation, have that conversation with a healthcare provider who knows your individual situation. The goal isn’t to dismiss emerging science—it’s to engage with it honestly while acting on what we actually know works.
Further Reading
Explore more articles related to this topic:
- NMN for Brain Fog: How Boosting NAD+ Crosses the Blood-Brain Barrier
- NMN for Brain Fog: Exploring Its Role in Cognitive Function
- NMN and Heart Health: Can It Reduce Arterial Stiffness and Blood Pressure?
- NMN for Weight Loss 2026: Does Boosting NAD+ Actually Burn Fat?
- NMN and Coffee: Does Caffeine Synergize or Interfere with NAD+ Production?
- NMN for Eye Health: Can It Protect Against Macular Degeneration and Vision Loss?
- The 12 Hallmarks of Aging Explained: A Beginner’s Guide to Longevity Science